UnitedHealthcare Deploys AI 'Avery' Amid AI Ethics Scrutiny
- 6.5 million members with employer-sponsored plans and 160,000 Medicare Advantage members initially have access to Avery
- 90% of interactions with Avery are resolved without needing human assistance
- $1.6 billion invested in AI by UnitedHealth Group in 2026
Experts emphasize that while Avery's AI-driven efficiency and scalability are promising, its success will hinge on robust ethical oversight, transparency, and proof that it enhances—not compromises—patient care and access.
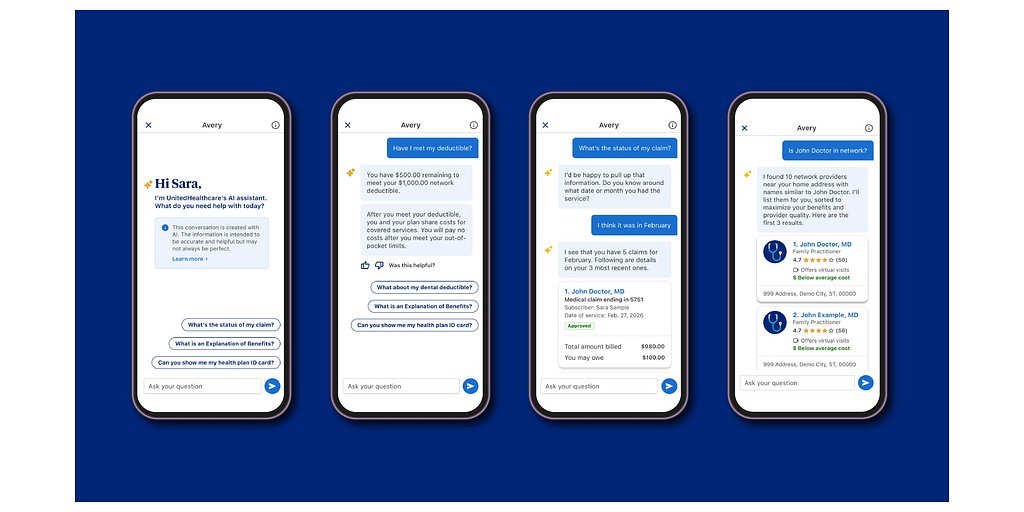
UnitedHealthcare Bets on AI Companion Amid Calls for Transparency
NEW YORK, NY – March 26, 2026 – UnitedHealthcare has launched "Avery," a generative AI companion designed to act as a personal health care navigator for millions of its members. The insurer, a division of the massive UnitedHealth Group, is positioning the tool as a solution to the notoriously complex American healthcare system, promising a simpler, more personalized experience.
The rollout comes as the industry accelerates its adoption of artificial intelligence, but also in the shadow of recent controversies that have placed the use of algorithms in healthcare under intense scrutiny.
A New AI Navigator for a Complex System
Available through the UnitedHealthcare app and website, Avery is designed to provide members with a single, unified point of contact for a wide array of needs. The AI can answer questions about coverage and benefits, estimate costs for procedures, help find in-network providers, and even call and schedule appointments with primary care physicians on a member’s behalf.
“People want health care to be easier to use and tailored to their personal needs,” said Dan Kueter, CEO for UnitedHealthcare’s commercial business, in a statement accompanying the launch. “Avery is one way we are responding to consumer demand for a more coordinated and simpler experience and enabling our members to focus on what matters most: getting and staying well.”
The company reports that Avery learns from user interactions to tailor its responses, adapting to an individual’s specific health plan and demographics. The tool is initially available to 6.5 million members with employer-sponsored plans and 160,000 Medicare Advantage members, with an aggressive expansion planned to reach over 20 million members by the end of the year.
UnitedHealthcare claims a high rate of efficacy, stating that in 90% of interactions, members using Avery have their needs met without needing to speak to a human representative. This self-service capability is central to the company's goal of reducing administrative friction for both patients and its own operations.
Innovation Amidst Scrutiny: The Ethics of AI in Healthcare
While promoting Avery's potential, UnitedHealthcare is also taking pains to address the significant ethical and privacy concerns surrounding AI in the health sector. The company states that Avery and its other AI tools operate within "rigorous oversight and governance frameworks designed to ensure safety, fairness and privacy with human expertise guiding output."
According to the company's Responsible AI program, its models do not store member data, make final coverage decisions, or replace clinical judgment. This distinction is critical, as UnitedHealth Group has faced legal and public backlash over its past use of AI.
In late 2024, a widely reported lawsuit alleged that a different algorithm used by the company, known as "nH Predict," was wrongfully denying post-acute care for elderly Medicare Advantage patients. The suit claimed the tool, which had a reported 90% error rate, was overriding physicians' recommendations to prematurely end care, raising questions about whether cost-cutting was prioritized over patient well-being.
Though UnitedHealthcare insists that Avery is fundamentally different and does not make clinical or coverage determinations, the legacy of the nH Predict controversy casts a long shadow. Privacy advocates and healthcare watchdogs will be closely monitoring Avery's rollout for transparency, fairness, and its true impact on patient access to care, demanding proof that its internal governance is robust enough to prevent similar issues.
The Evolving Role of the Human Advocate
Beyond the member-facing experience, UnitedHealthcare is framing Avery as a powerful tool for its own workforce. The company's narrative emphasizes augmentation over replacement, suggesting the AI will empower human customer advocates rather than render them obsolete.
When a member’s query is too complex for Avery or when a live conversation is requested, the system is designed to seamlessly transfer the member to a human advocate. Crucially, the AI provides the advocate with a full synopsis of the interaction, eliminating the common frustration of members having to repeat their story and details.
By automating routine administrative tasks like taking notes and searching for basic information, Avery is intended to free up advocates to concentrate on more complex, high-stakes member issues that require empathy and nuanced problem-solving. This model represents a potential future for customer service, where AI handles the volume of simple queries, allowing human experts to function as high-level case managers. However, with a 90% self-service rate, questions remain about the long-term impact on the size and structure of the customer service workforce and the skills that will be required for these evolving roles.
A Competitive Push in a Tech-Driven Market
The launch of Avery is not happening in a vacuum. It represents a significant move in the escalating technological arms race among major health insurers. UnitedHealth Group has committed to investing a staggering $1.6 billion in AI this year alone, with Avery being just one of more than 1,000 AI solutions deployed across its vast enterprise.
Other major players are making similar investments. Humana, for instance, recently deployed "Agent Assist," a staff-facing AI tool developed with Google Cloud to help its own advocates manage calls more efficiently. While Humana's tool is internal, Avery's direct-to-consumer approach signals UnitedHealthcare's ambition to lead in member-facing technology.
This aggressive push into AI is seen by industry analysts as a strategic imperative for insurers grappling with rising healthcare costs and consumer demand for digital convenience. By streamlining navigation and administrative processes, these tools promise not only a better member experience but also significant operational efficiencies. As these technologies evolve, their ability to deliver on the dual promises of improved care access and cost containment will be the ultimate measure of their success, setting the standard for the future of the health insurance industry.
