AI vs. AI: Why Your Heart Monitor Still Cries Wolf, and How to Fix It
- 32.9% of AI-equipped ICM alerts are non-actionable, meaning they don't require clinical intervention.
- 46.8% of false cardiac 'pause' alerts caused by R-wave undersensing—a detection failure in devices.
- Implicity's AI improved specificity to 61.6% in AI-equipped devices, reducing false alarms while maintaining high sensitivity (98.3% for clinically meaningful arrhythmias).
Experts agree that while AI in cardiac monitors has improved detection, false alarms remain a major challenge, and standardized AI solutions like Implicity's ILR ECG Analyzer could significantly enhance accuracy and efficiency in remote cardiac care.
AI vs. AI: Why Your Heart Monitor Still Cries Wolf, and How to Fix It
CAMBRIDGE, Mass. – April 14, 2026 – For the millions of people living with implantable cardiac monitors (ICMs), the promise of the technology is constant vigilance and peace of mind. For their doctors, however, it has often meant a relentless barrage of data and a deluge of false alarms. New research presented at the 2026 European Heart Rhythm Association (EHRA) Congress reveals that even as device manufacturers have integrated artificial intelligence into their monitors, the problem of non-actionable alerts persists, creating a significant burden on clinical staff. The findings, presented by digital health leader Implicity, not only diagnose the root cause of this “alert fatigue” but also propose a novel solution: fighting AI with smarter, more standardized AI.
The Persistent Problem of False Positives
At the heart of the issue is a surprisingly high rate of false alarms. A landmark cross-manufacturer analysis presented by Implicity examined 2,659 rhythm episodes from 1,710 patients with ICMs from major manufacturers including Medtronic, Biotronik, Abbott, and Boston Scientific. The results were stark. Even in modern devices equipped with proprietary AI algorithms designed to filter out noise, nearly one-third (32.9%) of all flagged episodes were ultimately deemed non-actionable, meaning they did not require any clinical intervention. Another 30.6% were classified as “indeterminate.” For older devices without built-in AI, the numbers were even worse, with 45.4% of alerts being non-actionable.
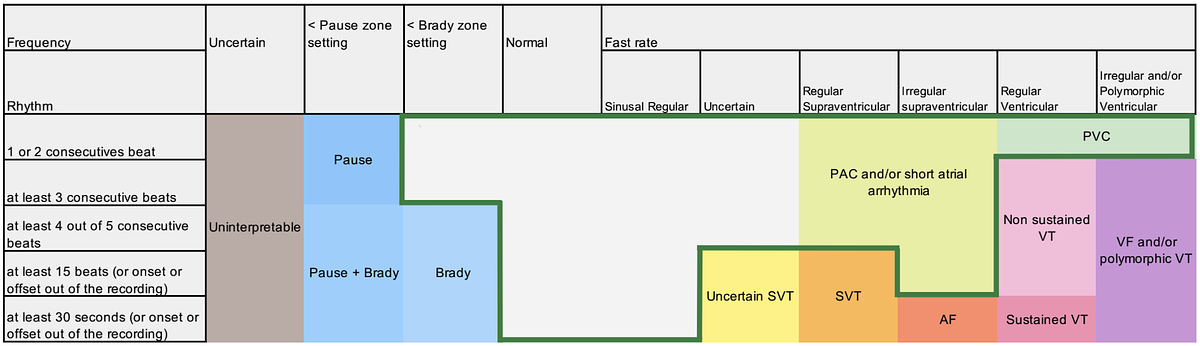
These are not just abstract percentages; each one represents a clinical event that a cardiologist or technician must manually review, consuming valuable time and resources. The research, which used an independent expert adjudication committee to apply a standardized framework based on international electrophysiology guidelines, pinpointed two key culprits behind this digital noise. First, a gap exists between how device algorithms interpret heart rhythms and how they are defined by clinical guidelines. This divergence can cause benign events, like premature ventricular contractions, to be mislabeled as serious arrhythmias. Second, fundamental signal-detection issues contribute significantly. The study found that alerts for cardiac “pause” events were a major driver of false positives, with a staggering 46.8% of them caused by R-wave undersensing—a phenomenon where the device simply fails to detect a heartbeat and incorrectly flags the resulting gap as a dangerous pause.
“False-positive alerts remain one of the biggest operational challenges in remote cardiac monitoring,” said Niraj Varma, MD, PhD, Professor of Medicine and Consultant Electrophysiologist at the Cleveland Clinic, in a statement accompanying the research. “Every episode flagged by an implantable cardiac monitor must be reviewed by a clinician, yet even devices equipped with manufacturer AI algorithms still generate a substantial number of non-actionable alerts. When interpretation varies across device platforms and guideline definitions are not consistently applied, it becomes more difficult for physicians to quickly determine which events truly require clinical attention.”
A Universal Translator for Cardiac Data
In response to this challenge, Implicity’s second study presented at EHRA evaluated a new approach: adding a universal, cloud-based AI layer on top of existing device data. This software, the Implicity™ ILR ECG Analyzer, is designed to act as a vendor-agnostic “universal translator,” analyzing transmissions from multiple manufacturer platforms through a single, standardized, guideline-based lens.
The results suggest this approach could be a breakthrough in solving the false-positive epidemic. The study showed that Implicity's AI algorithm maintained exceptionally high sensitivity, correctly identifying 98.3% of clinically meaningful arrhythmias in AI-equipped devices and 94.3% in non-AI models. In medicine, high sensitivity is critical—it means the system is highly effective at catching true problems and not missing critical events.
Crucially, it achieved this while dramatically improving specificity—the ability to correctly identify non-events. The algorithm achieved specificity of 61.6% in AI-equipped devices and 75.6% in non-AI models, effectively filtering out a massive portion of the noise that currently plagues clinicians. The system’s positive predictive value, or the probability that a positive alert represents a true arrhythmia, held steady at an impressive 74% across all device types. This demonstrates a reliable diagnostic performance that clinicians can trust, regardless of the underlying hardware.
This cross-platform capability represents a significant step toward standardizing cardiac care. Instead of grappling with the quirks and varying definitions of each manufacturer's proprietary software, hospitals and clinics can use a single system to normalize data. This not only improves efficiency but also pushes the industry toward greater interoperability, breaking down the data silos that have long complicated digital health.
From Data Overload to Patient-Focused Care
The implications of this technological advance extend far beyond the data itself, promising to reshape clinical workflows and improve patient care. The primary benefit is the potential to alleviate the immense review burden and subsequent burnout among cardiology staff. By intelligently filtering out tens of thousands of false alerts, the system allows highly trained professionals to stop managing data and start focusing on managing patients.
This efficiency gain has a direct economic impact. Clinics can potentially double their remote monitoring capacity without hiring additional staff, making these life-saving programs more scalable and sustainable. For health systems, this translates into significant cost savings by optimizing the use of their most valuable resource: clinical expertise.
For the more than 110,000 patients already on Implicity's platform across 250 medical facilities, the ultimate benefit is better, more focused care. When clinicians are not overwhelmed by false alarms, they can respond more quickly to genuine emergencies. This improved accuracy means a lower chance of a serious event being lost in the noise and a greater likelihood of timely intervention, which can prevent hospitalizations and improve long-term outcomes. For patients and their families, this translates into something invaluable: the peace of mind that comes from knowing the technology watching over their heart is not just vigilant, but intelligent.
While the specific version of the ILR ECG Analyzer (V2) evaluated in the EHRA study is not yet FDA cleared, Implicity has a history of securing regulatory approval for its AI algorithms. The company, co-founded by electrophysiologist Dr. Arnaud Rosier, continues to build on its mission to transform remote monitoring. With further data expected at the upcoming Heart Rhythm Society (HRS) Scientific Sessions in Chicago, the cardiology community will be watching closely as this new layer of intelligence promises to finally deliver on the full potential of remote cardiac care.
