AI Tool Reads Tumors to Predict Lung Cancer Treatment Success
- 1,300+ CT scans analyzed from 682 patients with non-small cell lung cancer
- QVT score predicts immunotherapy success by analyzing tumor blood vessel structure
- High QVT score linked to poorer survival outcomes after immunotherapy
Experts agree that the QVT score offers a promising, AI-driven method to personalize lung cancer treatment by assessing tumor blood vessel structure, potentially improving patient outcomes and reducing ineffective therapies.
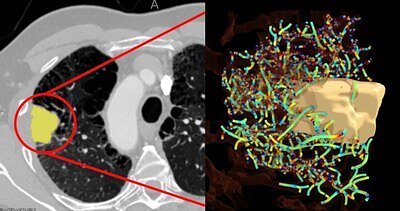
AI Tool Reads Tumors to Predict Lung Cancer Treatment Success
CLEVELAND, OH – March 10, 2026 – For the many lung cancer patients facing immunotherapy, a pivotal question looms: will this breakthrough treatment work for me? A new artificial intelligence tool may soon provide an answer earlier and more accurately than ever before by analyzing the very blood vessels that feed a tumor.
A multi-institutional study published in the Journal for ImmunoTherapy of Cancer details a new AI imaging biomarker, the Quantitative Vessel Tortuosity (QVT™) score, developed by Picture Health. By analyzing routine CT scans, the tool provides a powerful new metric that predicts patient outcomes and detects early signs of treatment response, potentially revolutionizing how oncologists personalize cancer care.
The large-scale study, which evaluated over 1,300 CT scans from 682 patients with non-small cell lung cancer across six medical centers, found that QVT could distinguish between patients who would likely benefit from immunotherapy and those who would not, addressing a critical gap in modern oncology.
The Limits of Current Prediction
Immunotherapy, which harnesses the body’s own immune system to fight cancer, has been a game-changer for non-small cell lung cancer. However, its success is not universal. The reality is that these powerful treatments are effective for only a subset of patients, leaving doctors with a significant challenge: how to identify the right candidates.
The current clinical standard for this decision is PD-L1 testing, which measures the level of a specific protein on tumor cells. While useful, PD-L1 is an imperfect predictor. Some patients with high PD-L1 levels don't respond to treatment, while others with low levels do. This variability can lead to patients enduring the potential side effects of an ineffective therapy or missing out on a treatment that could have worked.
"Immunotherapy has been a breakthrough for lung cancer, but the reality is it does not work for every patient," said Dr. Young Kwang Chae, the study's lead author and a Professor of Medicine at Northwestern University. This gap has spurred a search for more reliable biomarkers, pushing researchers to look beyond the tumor cell itself and into its surrounding environment.
A New Window into the Tumor Microenvironment
Picture Health's QVT score offers a novel approach by focusing on the tumor's vascular network—the complex web of blood vessels a tumor builds to supply itself with nutrients. These networks are often chaotic, tangled, and abnormal, which can create a barrier that prevents immune cells and cancer drugs from reaching the tumor.
The QVT technology uses AI to analyze over 900 different features of these blood vessels from a standard CT scan, something patients already receive as part of their routine care. It then distills this complex data into a single score that reflects the degree of vascular abnormality.
"We've known for decades that the blood vessels feeding a tumor contain important information about whether a patient is likely to benefit from treatment," Dr. Chae explained. "What's exciting is that we can now measure their structure using just a CT scan. This can allow us to personalize patient treatment, directing patients to their best care."
Researchers found that a high QVT score, indicating a more disorganized and chaotic vessel network, was independently associated with poorer survival outcomes after immunotherapy. Conversely, a low QVT score suggested a more normalized vascular structure, which correlated with a better prognosis. Crucially, the study also observed that early decreases in the QVT score during treatment—a sign that the blood vessels were normalizing in response to the therapy—appeared sooner than changes in tumor size, the traditional metric for assessing response.
"AI is allowing us to uncover hidden biological signals from medical images that were previously invisible to the human eye," noted Anant Madabhushi, PhD, Chief Scientific Officer at Picture Health. "By quantifying the architecture of tumor blood vessels from routine CT scans, QVT provides a new way to understand how a tumor is responding to treatment."
The Path to Clinical Adoption
The promise of AI-driven tools like the QVT score is immense, but the road from a published study to widespread clinical use is fraught with challenges. While the technology leverages existing hospital infrastructure—the CT scanner—its adoption hinges on clearing several significant hurdles.
First is the regulatory pathway. For the QVT score to be used in clinical decision-making in the United States, it will likely require clearance or approval from the Food and Drug Administration (FDA), a process that demands rigorous validation to prove its safety and effectiveness. While hundreds of AI-based medical imaging tools have been approved, each one must demonstrate its value and reliability.
Beyond regulation, a major barrier is integration into complex clinical workflows. For oncologists to adopt a new tool, it must be seamless to use and provide clear, actionable information without adding to their administrative burden. Physician trust is another critical factor. Many clinicians remain skeptical of "black-box" AI, where the tool's reasoning is not transparent. Building confidence requires not only robust validation but also education and tools that offer explainable insights.
Finally, there is the question of reimbursement. For hospitals to invest in and deploy new technologies, there must be a clear pathway for payment from insurers like Medicare and private companies. Without established billing codes and coverage policies, even the most groundbreaking innovations can stall.
Despite these challenges, the potential impact is driving significant interest. The findings are particularly timely as pharmaceutical companies increasingly explore combination therapies that pair immunotherapy with drugs targeting tumor blood vessels. Using QVT as a biomarker in clinical trials could help researchers more effectively identify patient subgroups most likely to benefit, potentially accelerating drug development. While this initial study focused on lung cancer, the underlying biology of abnormal tumor vasculature is common across many cancer types, suggesting the QVT score could one day help guide treatment decisions for a much wider range of patients.
