The Automated Eye: Tech Revolutionizes Neurocritical Care Assessment
- Inter-rater agreement between clinicians and automated pupillometers on pupil reactivity was only 33% in one study.
- The NPi score ranges from 0 to 4.9, with 3 or higher indicating a 'brisk' pupil.
- UT Southwestern's Clements University Hospital became the first to equip all Neuro ICU beds with automated pupillometer data integration into electronic medical records.
Experts in neurocritical care, including Dr. DaiWai M. Olson and Mary Kay Bader, advocate for the adoption of automated pupillometry as an objective, evidence-based tool to standardize neurologic monitoring and improve patient outcomes.
The Automated Eye: How Technology is Revolutionizing Neurocritical Care Assessment
SAN DIEGO, CA – May 13, 2026 – For generations, the simple penlight has been a staple of neurological exams, a quick way for clinicians to check a patient’s pupillary response. But in the high-stakes environment of critical care, where subtle changes can signal life-threatening emergencies, the subjectivity of this manual check is facing a technological reckoning. A new generation of automated pupillometers is replacing guesswork with objective data, and two of the nation's foremost neurocritical care nursing leaders are set to discuss this paradigm shift at a major industry conference.
At the upcoming American Association of Critical Care Nurses (AACN) National Teaching Institute & Critical Care Exposition in San Diego, Dr. DaiWai M. Olson and Mary Kay Bader, MSN, will lead educational sessions on the growing role of NPi® pupillometry. Hosted by medical technology company NeurOptics, the presentations will highlight how devices like the NPi-300 Pupillometer are transforming a fundamental bedside assessment, providing a level of precision and consistency previously unattainable.
This focus at the nation's largest gathering of critical care nurses underscores a significant movement in modern medicine: the push to standardize neurologic monitoring through evidence-based, objective tools. As hospitals increasingly adopt these technologies, the era of interpreting pupil size as “small, medium, or large” is giving way to a new standard of quantifiable, trendable data that empowers clinicians and can improve patient outcomes.
Beyond the Penlight: A New Standard in Neurological Assessment
The traditional pupillary light reflex exam, while foundational, is notoriously subjective. Different clinicians may interpret the same pupil's size and reactivity differently, and subtle changes can be easily missed, especially under the stressful conditions of an ICU. Research has highlighted this inconsistency; one study led by Dr. Olson found that inter-rater agreement between practitioners on pupil reactivity was only moderate, with clinicians and an automated pupillometer agreeing on a non-reactive pupil just one-third of the time.
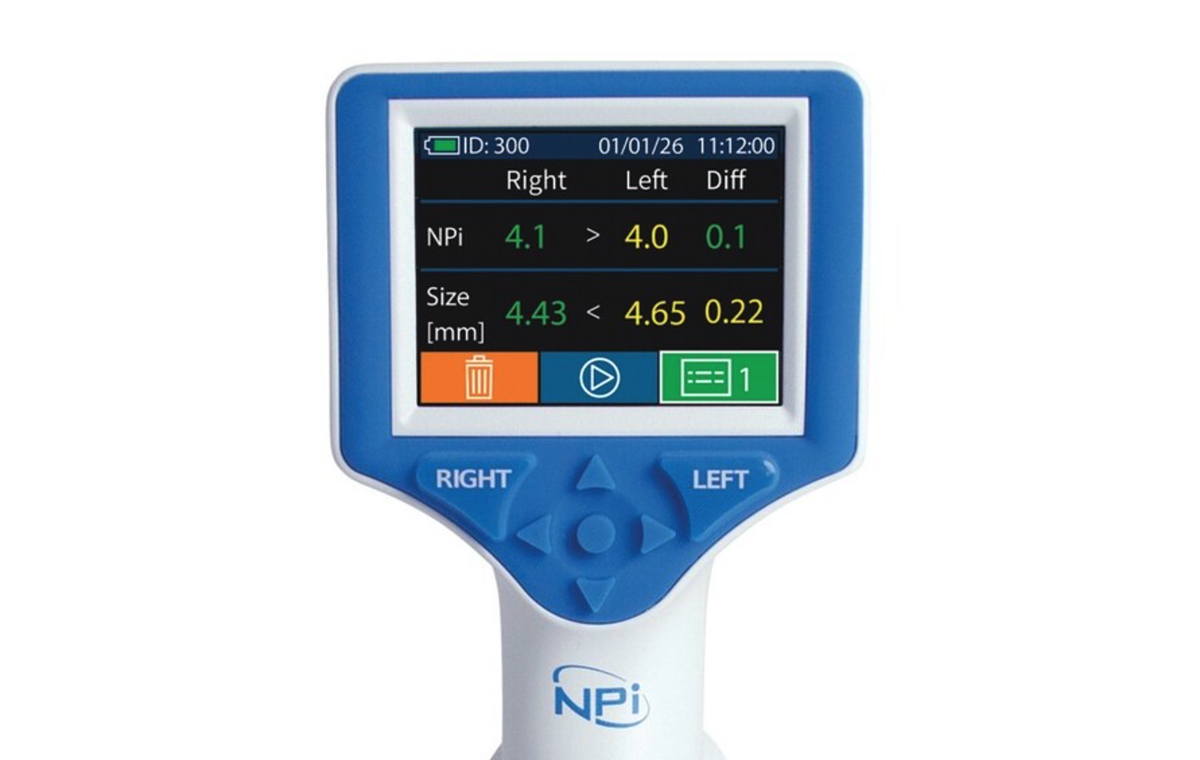
Automated pupillometry addresses this challenge directly. The NPi-300 Pupillometer, for example, uses an infrared camera and a calibrated light stimulus to provide precise, reliable measurements of pupil size, reactivity, and constriction velocity. Critically, it calculates the Neurological Pupil index™ (NPi), a proprietary score on a scale from 0 to 4.9. A score of 3 or higher indicates a “brisk” pupil, while scores below 3 signify sluggishness, and an NPi of 0 indicates a non-reactive pupil. This single, objective number removes ambiguity and allows for clear communication and documentation.
“Pupillary assessment is one of the key neurologic checks we can perform quickly and repeatedly at the bedside, but the traditional penlight exam has important limitations,” says Dr. Olson, a widely published nurse scientist. “NPi pupillometry gives clinicians an objective number they can trend, communicate, and use as part of a more consistent neurologic assessment.” This ability to trend data over time is crucial for early detection of neurological decline due to conditions like traumatic brain injury, stroke, or increased intracranial pressure.
Backed by Evidence and Leading Experts
The push for adoption is being championed by highly respected figures in the field. Dr. Olson, a Professor of Neurology and Neurosurgery at UT Southwestern Medical Center and Director of its Neuroscience Nursing Research Center, has been a pivotal force in building the evidence base for the technology. His work on the "Establishing Normative Data for Pupillometer Assessments in Neuroscience Intensive Care (END-PANIC)" registry is helping to create a global standard for pupillometer readings in neurologically impaired patients.
Joining him at the conference is Mary Kay Bader, a Neuroscience and Critical Care Clinical Nurse Specialist at Providence Mission Hospital and a recent recipient of the prestigious AACN 2026 Pioneering Spirit Award. With over four decades of experience and more than 70 publications, Bader has been instrumental in developing clinical protocols that integrate advanced technology into the care of critically ill patients. Her extensive experience and leadership roles, including past presidencies of both the Neurocritical Care Society (NCS) and the American Association of Neuroscience Nurses, lend significant weight to her advocacy for the technology.
“In critical care, change over time is often what matters most,” Bader notes. “When nurses can see pupillary trends clearly and document them consistently, that information can strengthen communication with the care team and support earlier recognition of potential neurologic change.” Their combined expertise and research form the bedrock of the educational sessions planned for the AACN conference, with Dr. Olson presenting on evidence-based practice and Bader focusing on clinical case studies.
From Research to Guideline: The Imperative for Objective Data
Perhaps the most compelling driver of adoption is the technology's formal recognition within clinical practice guidelines. The subjectivity of the manual exam has long been a known issue, and major medical bodies are now officially acknowledging automated pupillometry as a valuable tool. Recent guidelines from the American Heart Association (AHA), the Neurocritical Care Society (NCS), and the American College of Surgeons (ACS) have all cited the utility of NPi pupillometry in patient care.
This integration into guidelines for managing conditions like post-cardiac arrest care, trauma, and patients on extracorporeal membrane oxygenation (ECMO) marks a critical turning point. It signals to hospitals and clinicians that objective pupillary assessment is no longer a niche or experimental practice but is becoming an evidence-based imperative for high-quality care. For hospital quality improvement committees and administrators, these endorsements provide a clear mandate for investing in technologies that standardize care and enhance patient safety.
At UT Southwestern's Clements University Hospital, this future is already a reality. It became the first hospital in the world to equip all its Neuro ICU beds with an interface that automatically transfers pupillometer data into the electronic medical record. This level of integration not only ensures 100% data accuracy and real-time availability but also enables advanced analysis of trends, potentially reducing the need for frequent CT scans and the associated radiation exposure and costs.
As more critical care teams evaluate how to enhance their neurologic monitoring protocols, the sessions at AACN NTI 2026 offer a timely and practical guide. The presentations by Olson and Bader are designed for the frontline clinicians—nurses, specialists, and practitioners—who perform these vital assessments every day, providing them with the knowledge to interpret pupillary trends and integrate the technology into their workflows. NeurOptics' focus on in-booth education reflects a commitment to ensuring this powerful tool is not just adopted, but also expertly utilized to its full potential at the patient's bedside.
📝 This article is still being updated
Are you a relevant expert who could contribute your opinion or insights to this article? We'd love to hear from you. We will give you full credit for your contribution.
Contribute Your Expertise →