Peptilogics' Biofilm-Busting Drug Enters Pivotal Human Trial
- 2% of joint replacement surgeries result in prosthetic joint infections (PJI) due to biofilm formation.
- 7% failure rate in early PLG0206 trials vs. 35-55% with standard care.
- $20 billion annual economic burden from PJI in the U.S. alone.
Experts view PLG0206 as a promising first-in-class treatment for PJI, with potential to revolutionize care for medical device-related infections if trial results confirm its efficacy.
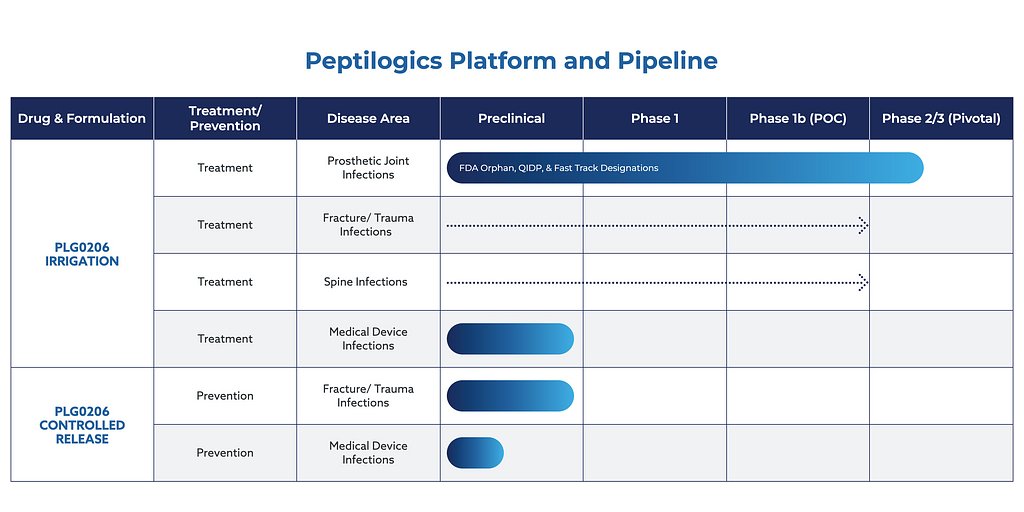
New Trial for Biofilm-Busting Drug Could Revolutionize Joint Infection Treatment
PITTSBURGH, PA – March 10, 2026 – A new clinical trial is offering a glimmer of hope against one of the most feared complications in modern medicine: the prosthetic joint infection. Pittsburgh-based Peptilogics has officially launched its pivotal RETAIN Phase 2/3 trial, enrolling its first patient to test a novel drug, PLG0206, designed to cure these devastating infections by attacking them at their source.
For the millions who undergo life-changing joint replacement surgery each year, the announcement marks a potential turning point in a battle that, until now, has been fought with brutal and often failing methods. The trial will evaluate if PLG0206 can provide a durable cure for prosthetic joint infections (PJI), a condition that carries a staggering economic burden and a mortality rate comparable to some forms of cancer.
The Brutal Reality of a Post-Surgical Nightmare
Each year, approximately five million people in the U.S., U.K., and Europe receive new joints. While overwhelmingly successful, a dark cloud hangs over these procedures: in about two percent of cases, bacteria colonize the implant and form a protective shield known as a biofilm. This slimy, resilient matrix makes the bacteria almost impervious to the body's immune system and traditional antibiotics, leading to a persistent, debilitating infection.
The current standard of care for PJI is a grueling ordeal. Most patients face a two-stage revision surgery, a process that involves removing the infected implant entirely, inserting a temporary, antibiotic-infused spacer, and enduring weeks or months of high-dose antibiotics. Only then, in a second major surgery, is a new prosthesis implanted. This physically and emotionally draining process has a failure rate between 15 and 25 percent and is associated with a shocking 25 percent five-year mortality rate. The financial toll is equally immense, contributing to an estimated $20 billion annual economic burden in the United States alone.
“Total joint arthroplasty is very successful in restoring function, mobility, and quality of life, but infection after joint replacement is a truly devastating complication that robs patients of that outcome and, in far too many cases, their lives,” said Javad Parvizi, MD, FRCS, Professor of Orthopedic Surgery at Acibadem University and past president of the American Association of Hip and Knee Surgeons.
A 'Biofilm Buster' Designed to Break the Siege
Peptilogics aims to change this grim calculus with PLG0206. The company describes the drug as a first-in-class, anti-biofilm therapeutic. Unlike conventional antibiotics that struggle to penetrate the biofilm fortress, PLG0206 is an engineered peptide specifically designed to breach this barrier and eradicate the persister bacteria hiding within.
“Biofilm is the root cause of medical device-related infections, and no approved therapy has ever been designed to target it,” said Jonathan Steckbeck, Ph.D., CEO of Peptilogics. “We built PLG0206 from the ground up as the first drug to penetrate biofilm and eradicate the persister bacteria protected by it.”
This approach has already shown remarkable promise in early studies. A Phase 1B trial demonstrated that among thirteen patients with PJI treated with PLG0206, only one experienced a recurrence of infection within 12 months—a seven percent failure rate. This stands in stark contrast to reported failure rates of 35 to 55 percent for the current standard of care in similar patient populations undergoing less invasive procedures.
A Fast-Tracked Strategy for a Multi-Billion Dollar Problem
The U.S. Food & Drug Administration (FDA) has already acknowledged the urgent need for a better solution. PLG0206 has received a trifecta of valuable regulatory incentives: Qualified Infectious Disease Product (QIDP), Orphan Drug, and Fast Track designations. These designations are reserved for treatments addressing serious, unmet medical needs and are designed to accelerate the development and review process.
Beyond expediency, these designations provide significant commercial advantages, including extended market exclusivity upon approval. The QIDP status alone adds five years of market protection, a powerful incentive for developing new antibiotics in a field that has seen dwindling investment. This strategic regulatory positioning has not only de-risked the development pathway but has also highlighted the drug's massive market potential for investors.
Peptilogics sees PJI as just the beginning. The company views PLG0206 as a potential platform technology. If successful, its biofilm-busting mechanism could be applied to a vast range of other medical device-related infections (MDRI) that plague modern healthcare. In the U.S. alone, an estimated 55 million people live with medical implants—from cardiovascular devices and spinal hardware to hernia mesh and vascular grafts—all of which are vulnerable to biofilm-driven infections.
The RETAIN Trial: The Ultimate Test
The RETAIN trial is a randomized, double-blind, placebo-controlled study, the gold standard in clinical research. It will enroll up to 240 patients with infected knee replacements across 50 clinical sites. Patients will undergo a procedure known as DAIR (Debridement, Antibiotics, and Implant Retention), where the joint is cleaned out but the original implant is kept. During this surgery, they will receive either PLG0206 or a placebo.
The primary measure of success will be the rate of treatment failure at 12 months. If PLG0206 can demonstrate a statistically significant improvement over the standard of care, it could fundamentally alter the treatment algorithm for PJI, potentially sparing thousands of patients from multiple surgeries and improving their chances of a full recovery.
As Dr. Parvizi noted, the trial is a landmark moment. “I’m excited about the promise of PLG0206 as a first-in-class treatment for patients with PJI, and as a potential solution for all medical device-related infections in the future.” For the countless patients living in fear of or suffering from these intractable infections, the results of this trial cannot come soon enough.
