Muscle Analysis Uncovers Hidden Mortality Risk in Kidney Disease
- 4.21x Higher Mortality Risk: Patients with adverse muscle composition (AMC) face a 4.21 times higher risk of death, even after adjusting for other factors.
- 30% of CKD Patients Affected: Nearly one-third of the study's CKD cohort exhibited AMC, highlighting its prevalence.
- 6.17x Unadjusted Risk: Initial data showed a 6.17 times higher mortality risk for those with AMC.
Experts conclude that muscle composition is an independent and critical predictor of mortality in chronic kidney disease, urging earlier interventions and personalized care strategies based on these findings.
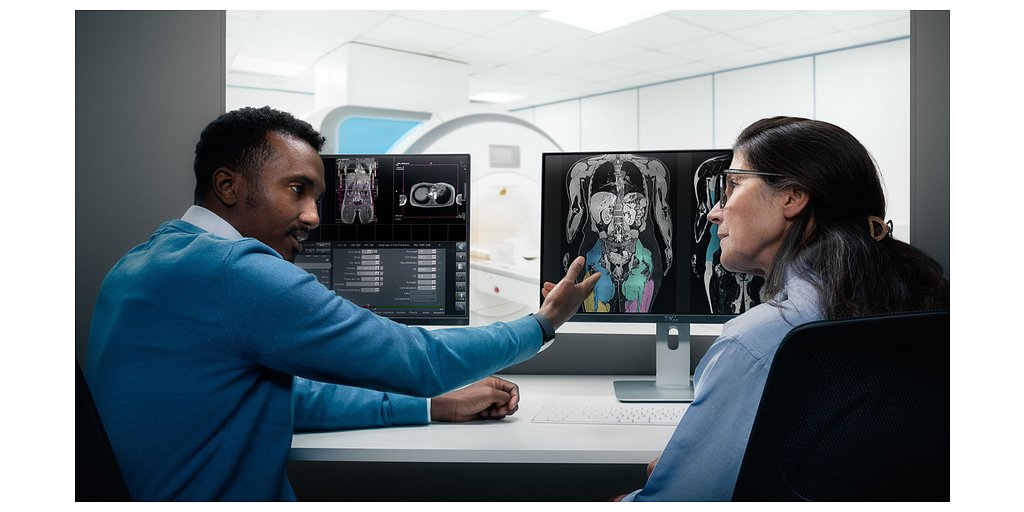
Muscle Analysis Uncovers Hidden Mortality Risk in Kidney Disease
LINKÖPING, Sweden – April 23, 2026 – A groundbreaking study is reshaping the understanding of risk in patients with chronic kidney disease (CKD), revealing that the composition of a person's muscles is a powerful and independent predictor of mortality. The research, spearheaded by health informatics leader AMRA Medical, demonstrates that individuals with what is termed "adverse muscle composition"—a combination of low muscle volume and high fat infiltration—face a more than four-fold increase in the risk of death.
Published in the prestigious Clinical Journal of the American Society of Nephrology, the findings leverage advanced magnetic resonance imaging (MRI) to look beyond traditional kidney function metrics. By providing a detailed, non-invasive assessment of muscle health, the technology uncovers a critical, previously underappreciated factor in patient outcomes, potentially paving the way for earlier interventions and more personalized care strategies for millions affected by CKD worldwide.
A New Marker for a High-Risk Population
The study, conducted in collaboration with researchers at Linköping University, analyzed data from 894 CKD participants in the UK Biobank imaging study. Using AMRA’s proprietary MRI-based analysis, the researchers precisely quantified thigh muscle volume and the degree of muscle fat infiltration (MFI). The results were stark: nearly one-third of the cohort exhibited adverse muscle composition (AMC).
Over a mean follow-up period of 3.6 years, individuals with AMC had a significantly higher rate of all-cause mortality. The initial unadjusted data showed a staggering 6.17 times higher risk. Even after researchers meticulously adjusted for a host of other factors—including age, gender, lifestyle choices, and established clinical markers of kidney disease—the association remained exceptionally strong, with a hazard ratio of 4.21.
This indicates that poor muscle quality is not merely a symptom of other underlying problems but an independent risk factor in its own right. Unlike some risk markers that identify only small, niche subgroups, AMC was present in a large portion of the study population, highlighting its clinical relevance for broader risk stratification. This discovery allows clinicians to identify a substantial at-risk group that might otherwise be overlooked by conventional assessments focused solely on kidney function tests like eGFR or albuminuria.
Beyond the Kidney: Muscle as a Systemic Health Barometer
While the study's immediate implications are for nephrology, its findings are part of a larger paradigm shift in medicine that views muscle health as a crucial indicator of overall systemic well-being. AMRA Medical's research extends far beyond kidney disease, exploring the role of muscle composition across a spectrum of chronic conditions.
Similar analyses are being applied to metabolic dysfunction-associated steatotic liver disease (MASLD), heart failure, and end-stage liver disease (ESLD). This growing body of evidence suggests that the health of our muscles is intricately linked to metabolic function, inflammation, and the body's ability to withstand the stress of chronic illness. Poor muscle quality, often characterized by sarcopenia (age-related muscle loss) and increased fat infiltration, is increasingly seen not just as a consequence of disease but as a contributor to its progression and a predictor of poor outcomes.
This holistic view positions muscle composition as a fundamental biomarker. For the pharmaceutical industry, it opens up new avenues for therapeutic development. Instead of targeting a single organ in isolation, future treatments might focus on improving muscle health to build patient resilience and improve survival across multiple diseases. The ability to quantify muscle changes accurately provides drug developers with a powerful tool to measure the effectiveness of such systemic interventions in clinical trials.
The Promise and Hurdles of Precision Imaging
The technological foundation of this discovery is MRI-based body composition analysis, a method that offers a significant leap in precision compared to existing clinical tools. Traditional methods like Dual-energy X-ray Absorptiometry (DEXA) and bioelectrical impedance analysis (BIA) can be less reliable in CKD patients, as their accuracy is often compromised by the fluid shifts and hydration status common in kidney disease. Computed tomography (CT) can provide detailed images but involves radiation exposure.
AMRA's MRI-based platform, which has received FDA 510(k) clearance and a CE Mark in Europe, avoids these pitfalls. It provides a highly standardized, reproducible, and radiation-free analysis of fat and muscle tissue from a single, rapid scan. This "gold standard" approach generates detailed biomarkers, such as visceral fat volume and liver fat fraction, alongside muscle metrics, offering a comprehensive snapshot of a patient's metabolic health.
However, the path from a groundbreaking study to widespread clinical adoption is fraught with challenges. The primary barriers are cost and accessibility. MRI scans are significantly more expensive than DEXA or BIA, and the equipment is not available in every clinical setting. Furthermore, navigating the complex landscape of healthcare reimbursement is a major hurdle for any new diagnostic technology. Even with regulatory approval, securing payment codes from insurers and healthcare systems to cover the cost of the analysis is a slow and arduous process. Without clear reimbursement pathways, hospitals and clinics are often hesitant to invest in and adopt new technologies, regardless of their clinical potential.
Redefining Clinical Trials and the Future of Patient Care
Despite these systemic hurdles, the immediate impact of this research is being felt in the world of clinical research and drug development. The ability to precisely stratify patients based on a robust biomarker like AMC is invaluable for designing more efficient and targeted clinical trials. By enrolling patients with a clearly defined risk profile, researchers can better assess the efficacy of new interventions aimed at improving outcomes in CKD and other chronic diseases.
For patients, the long-term vision is a move toward truly personalized medicine. In the future, a CKD patient might undergo a rapid MRI scan as part of their routine assessment. The resulting report, detailing their specific muscle and fat composition, could empower their physician to recommend tailored interventions long before a critical decline occurs. This could range from specific nutritional plans and exercise regimens designed to combat muscle fat infiltration to new classes of drugs that target muscle health directly.
This data-driven approach promises to make chronic disease management more proactive and less reactive. By providing deep, actionable insights from within the body, advanced imaging technologies are helping to uncover the hidden connections between different organ systems and redefine what it means to be at risk. This research underscores that in the fight against chronic disease, the strength and quality of our muscles may be one of our most important, and until now, overlooked, allies.
📝 This article is still being updated
Are you a relevant expert who could contribute your opinion or insights to this article? We'd love to hear from you. We will give you full credit for your contribution.
Contribute Your Expertise →