Micro-Ultrasound: The New Guideline-Backed Force in Prostate Cancer Care
- 70-micron resolution: Micro-ultrasound offers 300% higher resolution than conventional ultrasound.
- 100+ peer-reviewed publications: Strong evidence base supporting the technology.
- NCCN guideline inclusion: Officially recognized as a key diagnostic tool in 2026.
Experts conclude that micro-ultrasound is a validated, guideline-supported alternative to MRI for prostate cancer diagnosis, offering improved accessibility and diagnostic accuracy.
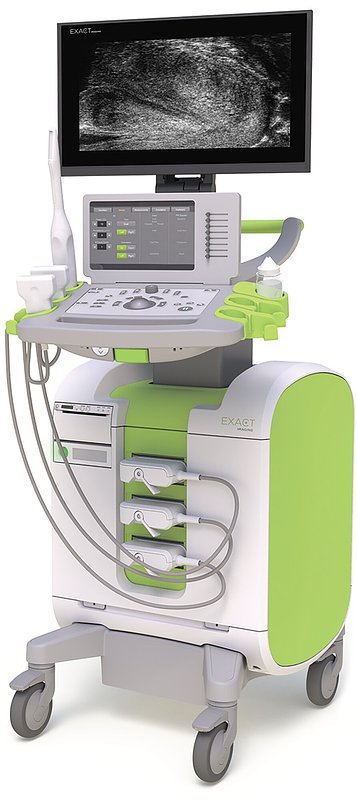
Micro-Ultrasound Earns Key Guideline Nod in Prostate Cancer Diagnosis
MARKHAM, Ontario – January 29, 2026 – A major shift is underway in the diagnosis of prostate cancer, as high-resolution micro-ultrasound has been officially recognized as a key diagnostic tool by one of the nation's leading cancer authorities. This development, validating a technology that offers a powerful alternative to MRI, promises to enhance diagnostic accuracy, improve patient access, and reshape the standard of care for millions of men.
A New Clinical Powerhouse: Guideline Inclusion and Robust Evidence
The National Comprehensive Cancer Network® (NCCN®), whose guidelines are a benchmark for oncology care worldwide, has included micro-ultrasound in its 2026 Clinical Practice Guidelines for the Early Detection of Prostate Cancer. The network recognized the technology as "non-inferior" to the current gold standard, multiparametric MRI (mpMRI) and mpMRI fusion-guided biopsy. This endorsement is not a minor update; it represents a pivotal moment for a technology that has been steadily building a formidable case for its efficacy.
This inclusion is built on a foundation of over 100 peer-reviewed publications. A landmark study published in the prestigious Journal of the American Medical Association (JAMA), known as the OPTIMUM trial, provided high-level evidence demonstrating that micro-ultrasound is just as effective as MRI-guided biopsies in detecting clinically significant prostate cancer.
For years, mpMRI has been the recommended step before a prostate biopsy, lauded for its ability to help urologists visualize suspicious lesions and reduce unnecessary procedures. However, the method is not without its drawbacks, including high costs, limited availability, inconsistent insurance reimbursement, and patient-specific contraindications such as claustrophobia or the presence of pacemakers and certain metal implants. The NCCN's recognition of micro-ultrasound provides clinicians and patients with a validated, guideline-supported alternative that addresses many of these challenges head-on.
The Technological Edge of 70-Micron Resolution
At the forefront of this innovation is Markham-based Exact Imaging and its ExactVu™ micro-ultrasound platform. The system operates at a frequency of 29 MHz, providing a real-time resolution of 70 microns—a level of detail nearly 300% higher than conventional ultrasound. This allows urologists to visualize prostate tissue and potential tumors with unprecedented clarity, directly in their office and in real time.
This high-resolution imaging enables clinicians to perform "targeted" biopsies with greater confidence, similar to the approach used with MRI fusion systems. Leading cancer centers have already integrated the technology into their clinical practice. At Fox Chase Cancer Center in Philadelphia, for example, the ExactVu system is utilized to provide more accurate biopsies, guide active surveillance for men with low-risk cancer, and serve patients who are ineligible for an MRI.
By providing an in-office solution, micro-ultrasound can streamline the diagnostic pathway. A patient can potentially undergo a high-resolution scan and a targeted biopsy in a single visit, reducing the anxiety, cost, and logistical complexity associated with scheduling separate appointments for an MRI scan and a subsequent fusion biopsy. The technology also features capabilities like FusionVu™, which allows for the integration of previously acquired MRI targets, offering clinicians the flexibility to combine the strengths of both imaging modalities.
Executing a Vision: From Clinical Validation to Commercial Dominance
Recognizing that clinical validation is only half the battle, Exact Imaging has been executing a shrewd commercial strategy to translate its technological advantage into market leadership. In a significant move, the company transitioned to a direct sales model in the United States in July 2025. This pivot allows for greater control over customer relationships, provides direct feedback for product improvement, and ensures that a highly specialized sales force can effectively communicate the technology's value to key decision-makers.
The strategy appears to be paying off. The company reports strong momentum, expanding its installed base across a diverse range of healthcare settings, including independent urology practices, major academic medical centers, and U.S. Department of Veterans Affairs facilities. This direct approach is complemented by an international growth strategy that leverages new distributor partnerships to increase system placements worldwide.
This dual focus on clinical excellence and commercial execution creates a powerful feedback loop. As more institutions adopt the technology, more data is generated, further strengthening the clinical evidence. This, in turn, fuels broader acceptance and drives demand, a cycle that the recent NCCN guideline inclusion is expected to accelerate significantly.
Reshaping the Future of Prostate Cancer Care
The implications of micro-ultrasound's ascent are profound, extending from the urologist's office to the patient's experience. For clinicians, it offers a powerful, accessible, and efficient tool that integrates seamlessly into their workflow.
"The inclusion of micro-ultrasound in NCCN’s internationally recognized guidelines reflects growing clinical confidence and provides urologists with a guideline-supported diagnostic option," noted Randy AuCoin, chief executive officer of Exact Imaging, in a recent statement. "We expect this recognition to further support adoption across a wide range of care settings."
For patients, the benefits are even more tangible. It means greater access to state-of-the-art diagnostics, a potentially faster and less fragmented path to a definitive diagnosis, and a viable high-quality option for those who cannot undergo an MRI. As the technology becomes more widespread, it could play a crucial role in not only detecting cancer earlier and more accurately but also in managing it more effectively through applications in active surveillance and the guidance of focal therapies. This evolution in diagnostic imaging is a critical step forward in the ongoing fight against prostate cancer, promising a future where care is more precise, accessible, and patient-centered.
