Liver Health: The Hidden Risk for Heart Failure in AFib Patients
- 7,543 adults aged 60+ with AFib studied over nearly a decade
- 30-40% of older adults globally affected by MASLD (Metabolic dysfunction-associated steatotic liver disease)
- Alcoholic liver disease (ALD) carries the highest risk of progressing to heart failure among SLD subtypes
Experts conclude that liver health, particularly steatotic liver disease (SLD), is an independent and graded predictor of heart failure risk in AFib patients, necessitating a more holistic approach to managing cardiometabolic health.
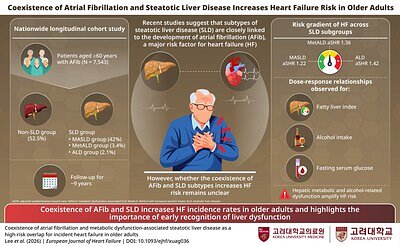
Liver Health: The Hidden Risk for Heart Failure in AFib Patients
SEOUL, South Korea – March 23, 2026 – For millions of older adults living with atrial fibrillation (AFib), the primary focus has long been on managing heart rhythm and preventing strokes. However, groundbreaking research from Korea University suggests a critical, and largely overlooked, risk factor for developing heart failure may reside in an entirely different organ: the liver.
A nationwide study has identified steatotic liver disease (SLD)—a spectrum of conditions characterized by excess fat in the liver—as a significant amplifier of heart failure risk in older adults with AFib. The findings, published in the European Journal of Heart Failure, establish a direct and graded link between liver health and cardiac vulnerability, signaling a potential paradigm shift in how clinicians assess and manage one of the world's most common heart conditions.
The Unseen Connection: A Deeper Look at the 'Liver-Heart Axis'
The Korean research team, led by Professor Seogsong Jeong, analyzed the health data of 7,543 adults aged 60 and older with AFib over nearly a decade. Their analysis revealed a clear and troubling pattern: individuals with any form of SLD faced a higher risk of developing heart failure compared to their counterparts with healthy livers.
More strikingly, the risk wasn't uniform. It followed a graded pattern depending on the subtype of liver disease, highlighting a compounding effect of metabolic dysfunction and alcohol consumption. The study categorized SLD into three main types:
- Metabolic dysfunction-associated steatotic liver disease (MASLD): This is the most common form, strongly linked to obesity, type 2 diabetes, and other metabolic risk factors. It was formerly known as non-alcoholic fatty liver disease (NAFLD) and affects an estimated 30-40% of older adults globally. Patients with MASLD had an elevated risk of heart failure.
- Metabolic dysfunction and alcohol-associated liver disease (MetALD): This category applies to individuals who meet the criteria for MASLD but also consume moderate amounts of alcohol. Their risk of heart failure was intermediate, higher than those with MASLD alone.
- Alcoholic liver disease (ALD): Caused by significant, chronic alcohol intake, this subtype carried the highest risk of progressing to heart failure.
These findings provide robust evidence for the growing importance of the “liver-heart axis,” a concept describing the intricate, bidirectional relationship between liver and cardiovascular health. A sick liver doesn't just stay sick; it can release inflammatory signals, disrupt lipid metabolism, and worsen insulin resistance throughout the body. These systemic effects create a hostile environment for the heart, promoting vascular stress and cardiac remodeling—processes that can accelerate the progression to heart failure, especially in a heart already strained by AFib.
Professor Jeong explained the study's rationale: "Fatty liver disease develops through different metabolic and alcohol-related pathways, and these differences may affect how AFib progresses to HF. Our study aimed to better understand this relationship."
A Growing Public Health Concern
The study's conclusions arrive at a critical moment. The global prevalence of the conditions that fuel SLD is skyrocketing. Obesity has nearly tripled worldwide since 1975, and metabolic syndrome—a cluster of conditions including high blood pressure, excess body fat around the waist, and high blood sugar—now affects up to a third of adults in many Western countries.
These trends are driving an epidemic of MASLD, which experts now call a systemic disease rather than just a liver ailment. The consensus among many hepatologists is that patients with SLD are more likely to die from cardiovascular events than from liver failure. The Korea University study adds a new layer of urgency to this reality, directly connecting the liver's metabolic state to outcomes in the world's most common cardiac arrhythmia.
Combined with the persistent public health challenge of harmful alcohol consumption, which drives ALD and contributes to MetALD, the stage is set for a potential surge in liver-related heart failure cases. This research suggests that as the population ages and these metabolic conditions become more common, the burden of heart failure among AFib patients could grow substantially unless the role of the liver is addressed.
Shifting the Paradigm in Clinical Practice
Perhaps the most significant implication of the study is its challenge to current clinical practice. Major cardiology guidelines from bodies like the American Heart Association and the European Society of Cardiology focus on traditional risk factors like hypertension, diabetes, and obesity when managing AFib. While these conditions are the root causes of MASLD, the liver itself is not explicitly considered a target for screening or a formal part of the risk calculation for heart failure.
This research argues for a more holistic view. By demonstrating that liver health is an independent and graded predictor of heart failure, the study suggests that cardiologists and primary care physicians may need to look beyond the heart to protect it. Incorporating liver-related metabolic signals into routine AFib reviews could allow for more refined risk stratification, helping to identify patients who need more intensive monitoring and intervention.
"Early detection and management of liver–metabolic dysfunction may help reduce the risk of HF in patients with AFib," concluded Professor Jeong. This could translate into earlier and more aggressive lifestyle counseling focused on weight management, diet, and alcohol reduction for at-risk patients.
In the future, a simple blood test or a non-invasive liver scan for an AFib patient could become as routine as checking cholesterol. Greater awareness of these liver-heart interactions may not only improve individual patient outcomes but also guide the development of integrated care models that treat cardiometabolic health as the single, interconnected system it truly is.
