AI Stethoscopes Boost Heart Disease Detection in Landmark NHS Trial
- 2.3-fold increase in heart failure detection
- 3.5-fold increase in atrial fibrillation detection
- 1.9-fold increase in valvular heart disease detection
Experts conclude that AI-powered stethoscopes significantly enhance early detection of heart conditions in primary care, offering a proven, practical tool for improving cardiovascular outcomes when integrated responsibly into clinical workflows.
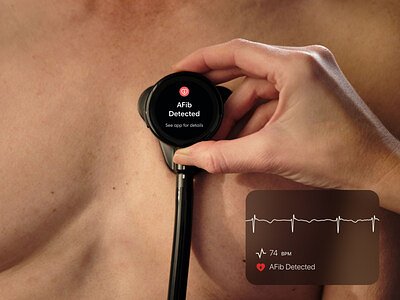
AI Stethoscopes Dramatically Boost Heart Disease Detection in NHS Trial
LONDON, UK – January 29, 2026 – A groundbreaking study published today in The Lancet has demonstrated that equipping primary care doctors with artificial intelligence-powered stethoscopes can dramatically increase the early detection of serious heart conditions. The landmark trial, one of the largest real-world evaluations of AI in medicine, signals a pivotal moment for integrating advanced technology into routine patient care.
The study, known as TRICORDER, found that when clinicians in the UK's National Health Service (NHS) used an AI-enabled digital stethoscope from Eko Health, the detection of heart failure increased 2.3-fold. The results were even more striking for atrial fibrillation, a common heart rhythm disorder that can lead to stroke, with a 3.5-fold increase in detection. Identification of significant valvular heart disease also rose by a factor of 1.9 compared to standard practice over a 12-month period.
This innovation represents a significant leap for one of medicine's most iconic tools, suggesting that AI can provide general practitioners (GPs) with a powerful early warning system for cardiovascular disease, long before patients might otherwise end up in an emergency room.
The Stethoscope, Reimagined: A Landmark Real-World Trial
Led by the Health Impact Lab at Imperial College London, the TRICORDER study was designed to test the AI's effectiveness not in a controlled laboratory, but within the busy and unpredictable environment of everyday primary care. The pragmatic, randomized trial involved 205 NHS general practices caring for a population of 1.5 million patients, with nearly 1,000 clinicians participating.
Practices were randomly assigned to either use the AI-enabled stethoscopes during routine appointments or continue with standard care. Eko Health's device functions like a traditional stethoscope but also captures high-fidelity heart sounds and an electrocardiogram (ECG) signal. Within seconds, a cloud-based AI algorithm analyzes the data for signs of structural or electrical abnormalities.
The study's scale and real-world design are what make its findings so compelling for the medical community. It provides rare, high-quality evidence that AI can be seamlessly integrated into existing clinical workflows to produce meaningful improvements in diagnostic yield.
"The Lancet publication of the TRICORDER study underscores the clinical importance and real-world impact of this technology," said Dr. Nicholas S. Peters, Professor of Cardiology at Imperial College London and a lead researcher on the study. "The stethoscope has always symbolized medicine's human touch. This innovation restores that connection while giving clinicians a powerful new ability to uncover heart disease at the point of care. The findings affirm that AI can be safely implemented in everyday practice to improve population-level outcomes."
Beyond the Numbers: Public Health and Economic Impact
The implications of catching these conditions earlier are profound. Heart disease remains a leading cause of death worldwide, and many diagnoses are made late, often during a costly and life-threatening emergency hospital admission. In the UK, heart failure alone consumes an estimated 4% of the entire NHS budget, with diagnoses made during emergency visits associated with higher costs and poorer patient survival.
By identifying at-risk patients in a GP's office, the technology offers a path toward proactive, preventative care. Earlier detection of atrial fibrillation allows for timely intervention with blood thinners to prevent strokes. Identifying valvular disease before symptoms become severe can lead to monitoring and treatment that averts the need for more complex surgery later. Research connected to the trial suggests that this approach could save the health system approximately £2,400 per patient by preventing emergency admissions for heart failure.
This shift represents a significant step towards alleviating the immense burden that cardiovascular disease places on healthcare systems. Rather than waiting for a crisis, AI-assisted tools empower primary care physicians to act as the first line of defense, efficiently triaging patients who need further specialist evaluation.
Paving the Way for AI in the Clinic
Publication in a prestigious, peer-reviewed journal like The Lancet provides the rigorous clinical validation that has often been the missing link for AI in healthcare. It moves the conversation from theoretical potential to proven utility, building trust among clinicians, regulators, and patients. Eko Health's device has already received regulatory clearance in the US from the FDA and UKCA marking in the United Kingdom, but large-scale evidence like the TRICORDER study is critical for driving widespread adoption.
However, experts caution that technology is only one piece of the puzzle. Successful integration requires careful planning, clear clinical guidelines, and ongoing education. While the AI provides a powerful signal, the ultimate diagnostic and treatment decisions rest with the clinician.
"It's a phenomenal assistive tool, but it will never replace the clinical judgment of an experienced physician," commented one cardiologist not involved in the study. "The key is using it to augment our skills, to hear things we might have missed, and to get the right patients to a specialist sooner. It's about enhancing expertise, not supplanting it."
This sentiment reflects a broader consensus that the "human-in-the-loop" model is essential for the responsible deployment of medical AI. The TRICORDER study itself supported clinicians with clear guidelines for how to act on the AI's findings, a crucial component of its success.
The Future of Primary Care Diagnostics
The market for AI-powered diagnostic tools is rapidly expanding, with several companies developing technologies to analyze everything from medical images to vital signs. The digital stethoscope space, in particular, is seeing intense innovation, with established players like 3M Littmann and specialized firms such as Thinklabs Medical and HD Medical also contributing to the field. This competition is driving advancements in algorithm sophistication and device integration, especially as telemedicine and remote patient monitoring become more common.
Despite the optimism, challenges remain. Ethicists and health tech experts point to the "black box" problem, where the inner workings of an AI algorithm can be opaque, making it difficult to understand its reasoning. There are also persistent concerns about data bias, where algorithms trained on non-diverse datasets could perform less accurately for certain populations, potentially exacerbating health inequities.
"We must ensure these powerful tools are rigorously tested across all demographic groups," noted a health policy analyst. "The goal is to reduce disparities in care, and that requires a conscious effort to prevent algorithmic bias from the outset."
Building patient trust is another critical hurdle. While clinicians may embrace the technology, patients may be wary of a diagnosis delivered by an algorithm. Transparency and clear communication about how these tools are used to support, not replace, their doctor's judgment will be paramount.
The TRICORDER study stands as a powerful testament to the potential of AI to revolutionize frontline medicine. By arming primary care physicians with enhanced senses, this new generation of smart stethoscopes is poised to make early cardiac detection more accessible, efficient, and effective, ultimately saving lives and reshaping the future of healthcare delivery.
