AI Slashes Prior Authorization Delays with 95% Clinician Approval
- 94.5% acceptance rate: Clinicians approved and submitted nearly 19 out of every 20 AI-generated prior authorization (PA) responses without modification.
- 95% of physicians: Believe PA-related delays negatively impact clinical outcomes.
- $23–$31 billion annually: Estimated cost of PA processes to the U.S. healthcare system.
Experts agree that AI-driven automation of prior authorizations significantly reduces administrative burdens, improves patient outcomes, and alleviates physician burnout, though concerns about data privacy and algorithmic fairness remain critical.
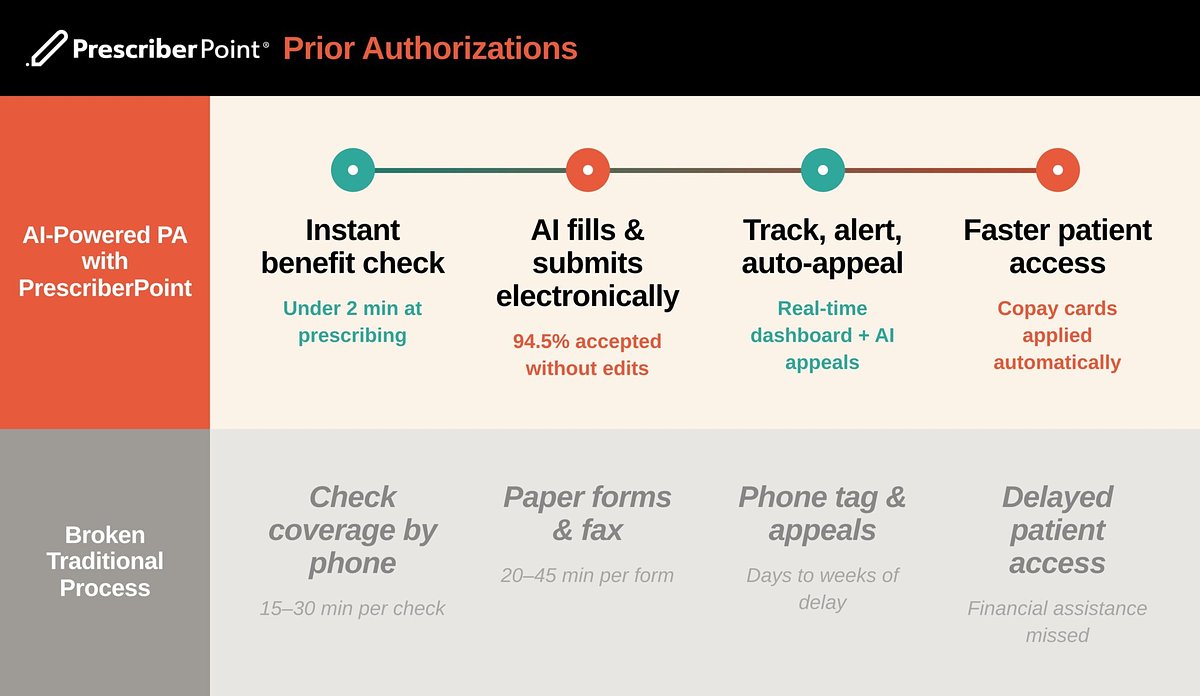
AI Slashes Prior Authorization Delays with 95% Clinician Approval
BOSTON, MA – April 21, 2026 – A new artificial intelligence solution is promising to dismantle one of the most significant barriers in American healthcare: the prior authorization (PA) process. PrescriberPoint, a Boston-based health technology company, has announced an AI agent that automates the entire PA lifecycle, boasting a 94.5% acceptance rate from clinicians in a recent study. The platform is demonstrating the potential to slash therapy start times from weeks to as little as 48 hours, a development that could have profound implications for patient outcomes and physician burnout.
The company's announcement is backed by a clinical validation study conducted at a weight management primary care practice. Over the course of the study, the AI processed 1,289 PA responses, with clinicians approving and submitting nearly 19 out of every 20 AI-generated answers without any modification. In one particularly demanding case for a specialty medication, the AI agent autonomously answered 163 distinct questions from an insurance payer, with the full submission accepted by the prescribing clinician.
"The PA process has been a black box — for prescribers, for patients, and especially for the brands whose therapies depend on getting through it," said Dan Cornwell, CEO of PrescriberPoint, in a statement. "Our AI agent doesn't just fill out forms. It understands what each payer requires, assembles the clinical evidence, and gets patients started on therapy faster."
Tackling Healthcare's Administrative Nightmare
Prior authorization, the requirement that physicians obtain pre-approval from payers for certain medications or procedures, has long been a source of friction and frustration. Intended as a cost-control measure, it has ballooned into a major administrative burden that industry experts estimate costs the U.S. healthcare system between $23 and $31 billion annually.
For frontline clinicians, the impact is felt daily. Physicians report spending an average of 12 hours per week navigating PA requirements, time that is diverted from direct patient care. This administrative load is a leading contributor to burnout, but its consequences extend directly to patient health. A staggering 95% of physicians surveyed in industry reports believe that PA-related delays have a negative impact on clinical outcomes. These delays can lead to treatment abandonment, disease progression, and in some cases, serious adverse health events as patients wait for necessary care.
The process often forces providers to engage in time-consuming back-and-forth communication with payers, digging through electronic medical records (EMRs) to find the specific clinical data required to justify a treatment. The complexity and opacity of different payer requirements can lead some providers to alter their prescribing habits altogether, either by choosing less effective but easier-to-approve medications or by modifying diagnoses simply to meet approval criteria.
A Proactive Approach to Automation
PrescriberPoint's solution aims to short-circuit this cycle of delays and rework by integrating directly into the physician's workflow at the point of prescribing. Unlike many existing PA solutions that are designed to handle "reactive" PAs—those that have already been rejected by a pharmacy—this platform works proactively. By sitting on the prescriber's side and connecting with the EMR, the AI triages the need for a PA the moment a prescription is written.
The AI agent leverages a vast repository of clinical and payer data to guide each submission. It performs real-time benefit checks to verify a patient's eligibility and reveal potential out-of-pocket costs. It then automatically populates the required documentation, translating complex payer questions into plain language for the clinician to review. The platform provides a clear dashboard to track the submission's progress and, if a denial occurs, automatically generates a structured appeal letter populated with relevant clinical documentation and arguments mapped specifically to the payer's denial reason.
This high degree of automation keeps the clinician in control but removes the manual drudgery. Patients are also kept in the loop through text message updates on PA status, pharmacy routing upon approval, and enrollment in copay savings programs, all without needing to download an app or create an account.
Pharma's New Playbook for Market Access
Beyond the clinical setting, the platform offers a significant strategic advantage to life sciences companies. For pharmaceutical brands, the PA process has historically been an opaque barrier, making it difficult to understand why prescriptions are abandoned or why access varies so widely across different payers and plans. This lack of visibility hampers their ability to support both patients and prescribers.
PrescriberPoint is positioning its platform as a solution to this problem, providing pharmaceutical partners with unprecedented insight into the patient access journey. By analyzing aggregated, anonymized data, brands can identify common hurdles, understand payer-specific requirements, and see where their therapies encounter the most resistance. This enables them to develop more effective market access strategies and provide prescribers with targeted resources at the exact moment a treatment decision is being made.
This model appears central to the company's business strategy. By offering its powerful tools to a network of what it reports as over 5 million healthcare professionals, PrescriberPoint creates a direct channel for pharmaceutical companies to reduce access barriers and measure the impact of their support programs on therapy adoption. The company is actively courting these partnerships and will be demonstrating its capabilities at the upcoming Asembia AXS26 Specialty Pharmacy Summit.
The Evolving Landscape of AI in Healthcare
The push to automate prior authorizations is part of a broader trend across the healthcare industry. Other companies and health systems have launched pilots using AI to streamline PA submissions, often with a human coordinator making the final judgment. However, PrescriberPoint's claim of automating the full PA lifecycle in a proactive manner represents a significant step forward.
This rapid technological advancement is occurring within a complex regulatory and ethical framework. The Centers for Medicare & Medicaid Services (CMS) has already issued rules to promote interoperability and streamline PA processes, signaling a federal push for the very standardization that makes such AI tools more effective. However, the use of AI to handle sensitive patient data raises critical questions about data privacy under HIPAA, the potential for algorithms to perpetuate existing biases in care, and the need for transparency in how automated decisions are made.
While PrescriberPoint's model emphasizes clinician oversight—the 94.5% acceptance rate highlights that a human is still the final arbiter—the increasing autonomy of these systems brings questions of accountability to the forefront. As these technologies become more deeply embedded in clinical practice, ensuring they are fair, secure, and transparent will be paramount for earning the trust of providers, payers, and patients alike.
📝 This article is still being updated
Are you a relevant expert who could contribute your opinion or insights to this article? We'd love to hear from you. We will give you full credit for your contribution.
Contribute Your Expertise →