AI Safety Net Aims to Catch Life-Threatening Missed Diagnoses
- 31% of imaging studies in acute care settings contain incidental findings.
- 83% of patients with significant incidental findings do not receive recommended follow-up care.
- 10-week pilot study reviewed 4,400 imaging studies, identifying 1,000 findings and triggering outreach for 259 moderate-to-high-risk cases.
Experts agree that AI solutions like Vital Guard can significantly improve patient safety by reducing missed diagnoses and ensuring critical follow-up care, though challenges in integration, regulation, and ethical considerations remain.
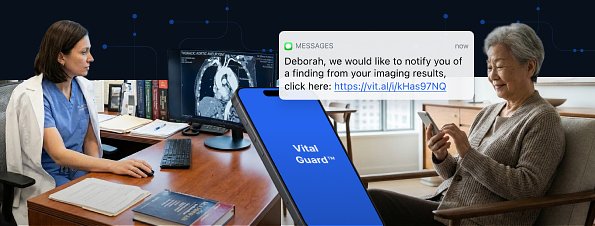
AI Safety Net Aims to Catch Life-Threatening Missed Diagnoses
CLAYMONT, Del. – February 25, 2026
A 73-year-old woman visited the emergency room for one issue, but a routine imaging scan revealed another, far more dangerous one: a thoracic aortic aneurysm. She left the hospital unaware of the ticking clock inside her. This dangerous communication gap is a common blind spot in modern healthcare, but a new technology aims to provide a digital safety net. Vital, a patient experience technology company, today announced the launch of Vital Guard™, an artificial intelligence solution that scans medical records to find and flag these overlooked, potentially life-threatening "incidental findings."
The Peril of Overlooked Findings
What happened to the 73-year-old woman is not an isolated incident. These discoveries, known as incidental findings (IFs), are abnormalities detected on imaging studies ordered for an unrelated reason. While many are benign, some can be the first sign of cancer, aneurysms, or other serious diseases. Research has shown that up to 31% of all imaging studies in acute care settings contain such a finding. The real breakdown, however, occurs after the discovery. An alarming 83% of patients with a significant incidental finding never receive the recommended follow-up care, a gap that can lead to delayed diagnoses, preventable harm, and significant legal exposure for hospitals.
"Incidental findings represent one of the most common and most preventable breakdowns in patient communication today," said Justin Schrager, MD, founder and Chief Medical Officer at Vital, in the company's announcement. In the chaotic environment of an emergency department or hospital floor, a secondary finding on a scan can easily be lost in the shuffle as clinicians focus on the primary reason for the patient's visit. This systemic failure point highlights a critical need for more robust tracking and communication systems.
A Digital Watchdog for Patient Records
Vital Guard is designed to ensure these critical details don't fall through the cracks. The system integrates with a hospital's existing Electronic Health Record (EHR) and uses advanced natural language processing (NLP) to read radiology reports and physician notes. The AI is trained to identify when an incidental finding is documented but not communicated to the patient or scheduled for follow-up. When it detects such a discrepancy, it automatically generates a high-priority worklist for a designated clinical team.
The platform then helps close the communication loop, using automated text messages to prompt patients to engage and ensure they are aware of the need for further action. This allows a single clinician to manage follow-up across multiple hospital sites, turning a fragmented, manual process into a structured, asynchronous workflow. A 10-week pilot study at Mercy Gilbert Medical Center demonstrated the platform's potential, reviewing over 4,400 imaging studies, identifying more than 1,000 findings, and triggering direct patient outreach for 259 moderate-to-high-risk cases.
The Business Case for Closing the Loop
Beyond the clear patient safety benefits, implementing such a system presents a compelling business case for healthcare organizations. Missed diagnoses stemming from failed follow-up on incidental findings are a leading driver of malpractice litigation. By creating an automated, auditable trail of identification and communication, platforms like Vital Guard can significantly reduce a hospital's legal and operational risk.
The economic argument extends to revenue as well. By ensuring patients receive necessary follow-up care—such as specialist consultations, further imaging, or biopsies—hospitals can capture "downstream revenue" that would otherwise be lost. In an era of razor-thin hospital margins, optimizing these care pathways is not just good medicine; it's good business. This has spurred a growing market for AI solutions that address both clinical quality and financial stability, with other technology firms also developing tools to tackle this specific problem.
Navigating the Hurdles of AI in Healthcare
The promise of AI in medicine is immense, but its implementation is not without challenges. Integrating new technology with complex and often outdated EHR systems remains a significant technical and financial hurdle for many hospitals. Furthermore, any system that handles Protected Health Information (PHI) must navigate the stringent requirements of HIPAA, demanding robust security protocols and legal agreements with vendors.
The ethical implications are also profound. The potential for algorithmic bias, where an AI could perform differently for various patient populations based on biased training data, is a major concern for developers and regulators. The U.S. Food and Drug Administration (FDA) is actively developing its framework for "Software as a Medical Device" (SaMD), focusing on ensuring clinical validity, transparency, and safety, but the landscape of liability for AI-driven medical errors remains a complex and evolving legal gray area.
Despite these challenges, the real-world impact is already being felt. In one case highlighted by Vital, a 54-year-old man who went to the ED for back pain had a CT scan that incidentally revealed a left adrenal mass. He was unaware of the finding until contacted through the new system. After a text message and a call, he connected with his primary care physician and was referred to an endocrinologist for monitoring. In another recent case, the system identified a malignant kidney lesion that had not been mentioned to the patient in the ER, escalating it for immediate follow-up and enabling the patient to access life-saving oncology care without delay.
